Early Signs of Venous Insufficiency
Venous insufficiency is often dismissed by millions worldwide as normal signs of aging or fatigue. Categorized as a progressive vascular condition, it occurs when leg veins have difficulty efficiently pumping blood back to the heart. The result is pooling of blood in the lower extremities. Early intervention is always your best chance to slow the progression of any condition, including venous insufficiency. Consulting with a vascular & vein center can help you prevent serious complications and improve symptoms related to this ailment.
What is Venous Insufficiency?
Damage to your leg veins causes them to work improperly; when this happens, it is referred to as venous insufficiency. Damage to the valves in your legs causes blood to pool rather than flow back to your heart as it should. The buildup and increase in pressure can cause swelling and ulcers.
Causes
Venous insufficiency is the result of damage to the veins in your legs. This can be due to:
- Malformations in your legs from birth.
- Changes in your leg veins prevent them from functioning correctly.
- Other conditions that cause damage to leg veins include deep vein thrombosis.
Early Warning Signs
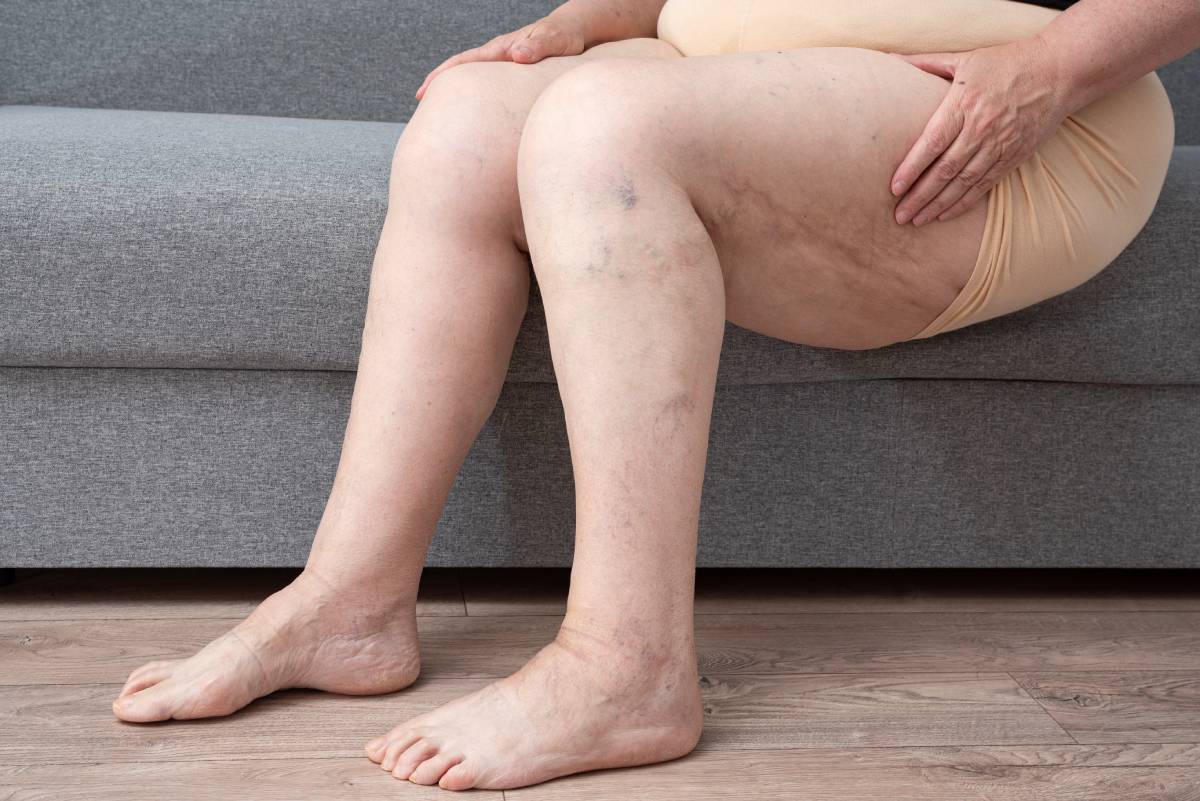
The earliest noticeable symptoms of venous insufficiency often appear on the skin’s surface. Spider veins, varicose veins, swelling, discoloration, and aches are all indicators of this vascular condition. If you experience any of these early signs, consider scheduling a visit with your physician.
Progressive Symptoms
As venous insufficiency progressively worsens, symptoms become more pronounced and life-affecting. Advanced stages bring more intense swelling, with your legs feeling tired and heavy, severely limiting your daily movement. Skin changes are more prominent and concerning. Pain increases from mild to persistent, and leg ulcers develop. Ulcers are a sign that you are experiencing severe venous insufficiency, which needs medical attention immediately. Minor injuries can lead to infection requiring aggressive vascular intervention.
Risk Factors and Prevention
The risk of venous insufficiency has several contributing factors. Anyone over the age of 50, of female gender, who is pregnant, or has a family history of venous insufficiency, is at an elevated risk of developing this condition. Obesity is another factor to consider, as it puts added pressure on your leg veins. Making relevant lifestyle modifications can help significantly reduce your risk and slow progression.
Treatment
The earlier venous insufficiency is detected, the less aggressive the treatment necessary. Immediately consult with a specialist if you begin to notice persistent leg swelling, varicose veins, discoloration in your legs, or chronic leg pain and heaviness. Modern vascular and vein centers offer diagnostic testing and can help you get appropriate treatment. Treatment can be as simple as lifestyle modifications and compression therapy, or as complex as phlebectomy.
Getting Ahead of Venous Insufficiency
Catching venous insufficiency early means less invasive treatment options and a greater chance of slowing its progression. This condition is highly treatable with modern medicine offering a wide range of minimally invasive options that help alleviate the symptoms by restoring proper blood flow in your leg veins. Persistent leg symptoms should never be ignored. If you are experiencing any of the early signs of venous insufficiency, schedule an appointment with an experienced vascular specialist for testing. Early intervention can help prevent complications and improve overall outcomes. Act early on warning signs and be sure to seek medical professionals with the credentials necessary to properly diagnose and treat venous insufficiency. It is never a good idea to gamble with your health, and gambling with venous insufficiency could leave you physically, mentally, and financially hurting.
Catch venous insufficiency early; consult with a vascular and vein center today.